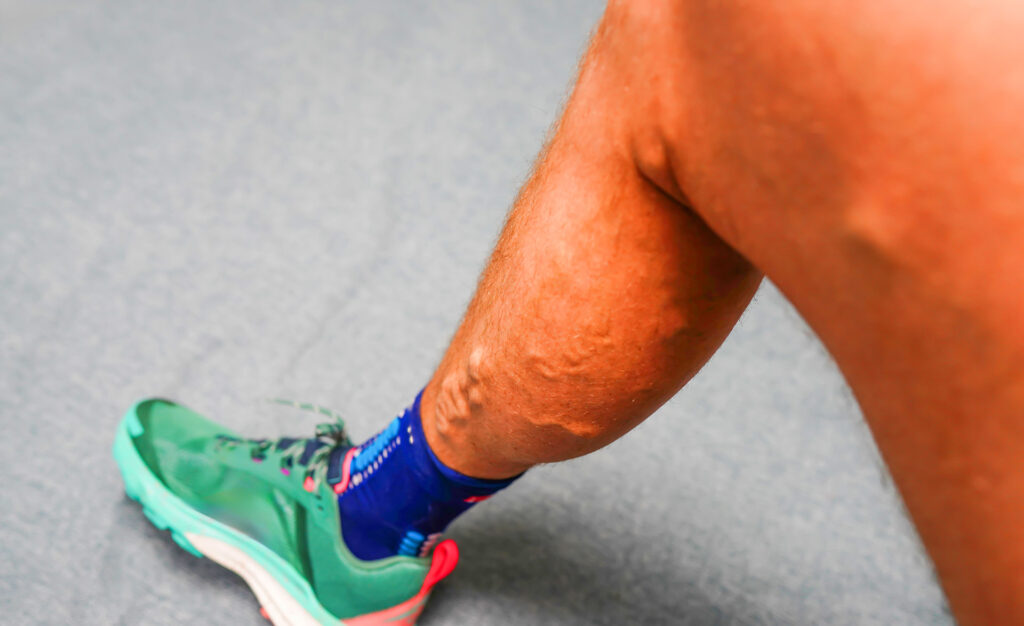
When healthy veins fail to function properly, a condition called venous insufficiency can develop. In more serious cases, it may be associated with complications such as deep vein thrombosis. This condition often appears as varicose veins, twisted, enlarged vessels that may look blue or purple beneath the skin.
These visible veins can form when the valves or vessel walls lose elasticity. Without proper function, blood is not efficiently returned to the heart and can begin to pool in the lower legs, leading to increased pressure and vein enlargement.
While some people view varicose veins as a cosmetic issue, others experience symptoms such as leg cramps, aching, heaviness, or fatigue.
These signs should not be ignored, as they may indicate an underlying circulation problem that warrants medical evaluation.

What Are the Hidden Dangers of Varicose Veins?
When varicose veins are left untreated, they can contribute to ongoing circulation problems and may be associated with more serious complications, including worsening venous insufficiency. Here are five critical dangers you should know about:
Edema (Fluid Retention and Swelling)
Increased pressure in damaged veins can cause fluid to leak from the bloodstream into surrounding tissues, leading to swelling (edema) in the lower legs and ankles. This fluid is typically clear or slightly yellow in appearance and may accumulate over time in the affected areas.
As the condition progresses, the skin can become discolored or feel firmer due to ongoing fluid retention and tissue changes.
In more severe cases, swelling may interfere with daily activities, including making it difficult to wear regular footwear or remain comfortable while standing or walking.
Varicose Eczema and Infection Risk
This skin condition can affect people with varicose veins, where stretched skin becomes dry, flaky, shiny, and intensely itchy. In some cases, red or purple patches and open sores called venous ulcers may develop on the lower legs, which can be signs of more advanced vein disease.
When the skin is affected by chronic swelling, its natural protective barrier can weaken. This may allow bacteria on the surface of the skin to enter deeper tissues, increasing the risk of infection such as cellulitis.
Symptoms of cellulitis can include fever, chills, nausea, vomiting, spreading redness, increasing pain, and sometimes reduced sensation in the affected area. If left untreated, the infection can worsen and may require urgent medical care, including more advanced treatment in severe cases.
Hemorrhage (Excessive Bleeding)
Varicose veins can act as areas where blood pools beneath the skin due to weakened or damaged vein valves. In some cases, even minor trauma to the affected area may lead to more noticeable bleeding than expected. Rarely, bleeding can also occur spontaneously, particularly when the skin and vein walls are fragile, and may be accompanied by other signs of advanced venous disease.
Some individuals first notice the problem when they see bleeding from the lower leg, which can sometimes be associated with dizziness or lightheadedness if the blood loss is significant. In severe cases, bleeding may be difficult to control and requires prompt medical attention.
Older adults may have a higher risk due to thinner skin and more fragile veins. Although uncommon, serious complications from ruptured varicose veins have been reported, highlighting the importance of seeking medical evaluation for advanced or worsening symptoms.
Thrombophlebitis and Deep Vein Thrombosis (Vein Inflammation with Clotting)
This condition involves inflammation in surface veins triggered by the formation of a blood clot, known medically as thrombophlebitis. Common symptoms include swelling, pain or tenderness in the affected area, redness of the skin, and reduced comfort or mobility.
Episodes of superficial thrombophlebitis typically last between two and six weeks. When associated with varicose veins, it may recur in some patients.
A more serious concern arises if the inflammation extends deeper. If a clot moves or spreads into the deep venous system, it can lead to deep vein thrombosis (DVT), which requires prompt medical evaluation.

Pulmonary Embolism (Life-Threatening Lung Blockage)
Recent research involving over 400,000 adults suggests that varicose veins may be associated with an increased risk of developing deep vein thrombosis (DVT).
DVT occurs when a blood clot forms in the deep veins, most commonly in the legs. Some individuals may experience symptoms such as pain, swelling, or edema in the lower legs, while others may have no noticeable signs.
The most serious risk arises if a clot dislodges and travels through the bloodstream. Blood from the legs returns to the heart and is then pumped into the lungs through the pulmonary arteries for oxygenation. If a clot becomes lodged in one of these arteries, it can block blood flow, reduce oxygen exchange, and lead to significant strain on vital organs. In severe cases, this condition can be life-threatening and requires urgent medical attention.

Available Treatment Options?
Pain during walking, sitting, or standing may be a sign of venous insufficiency and should not be ignored. The encouraging news is that effective, minimally invasive treatments are available. These modern vein treatments often with little to no downtime and, in many cases, coverage through health insurance depending on medical necessity.
The diagnostic process typically begins with an ultrasound performed by a vascular specialist trained to detect venous reflux, when the valves in the veins fail to circulate blood properly.
If reflux is confirmed, treatments such as radiofrequency ablation may be recommended. This non-surgical procedure uses controlled thermal energy to close the affected vein. Over time, the body naturally absorbs the sealed vein, and blood flow is redirected through healthier vessels, helping relieve symptoms.
If you are experiencing warning signs, early evaluation is important. Addressing varicose veins and venous insufficiency promptly may help reduce the risk of progression and related complications. Modern vein treatments have helped many patients improve comfort and leg function.
Frequently Asked Questions
Can varicose veins lead to blood clots?
Yes. Untreated varicose veins may contribute to thrombophlebitis, which is clot formation in surface veins. In some cases, this can extend into deeper veins and develop into deep vein thrombosis (DVT), a more serious condition.
Is bleeding from varicose veins dangerous?
It can be. Because varicose veins lie close to the skin, they may bleed significantly even with minor trauma. In rare cases, bleeding can occur spontaneously, particularly in older adults with fragile skin and vein walls, and may be difficult to control.
Are varicose vein treatments covered by insurance?
Often, yes. When varicose veins cause symptoms such as pain, swelling, or heaviness, treatments like radiofrequency ablation are commonly covered. Insurance approval is often supported by an ultrasound diagnosis confirming venous reflux.
Take control of your vein health now.