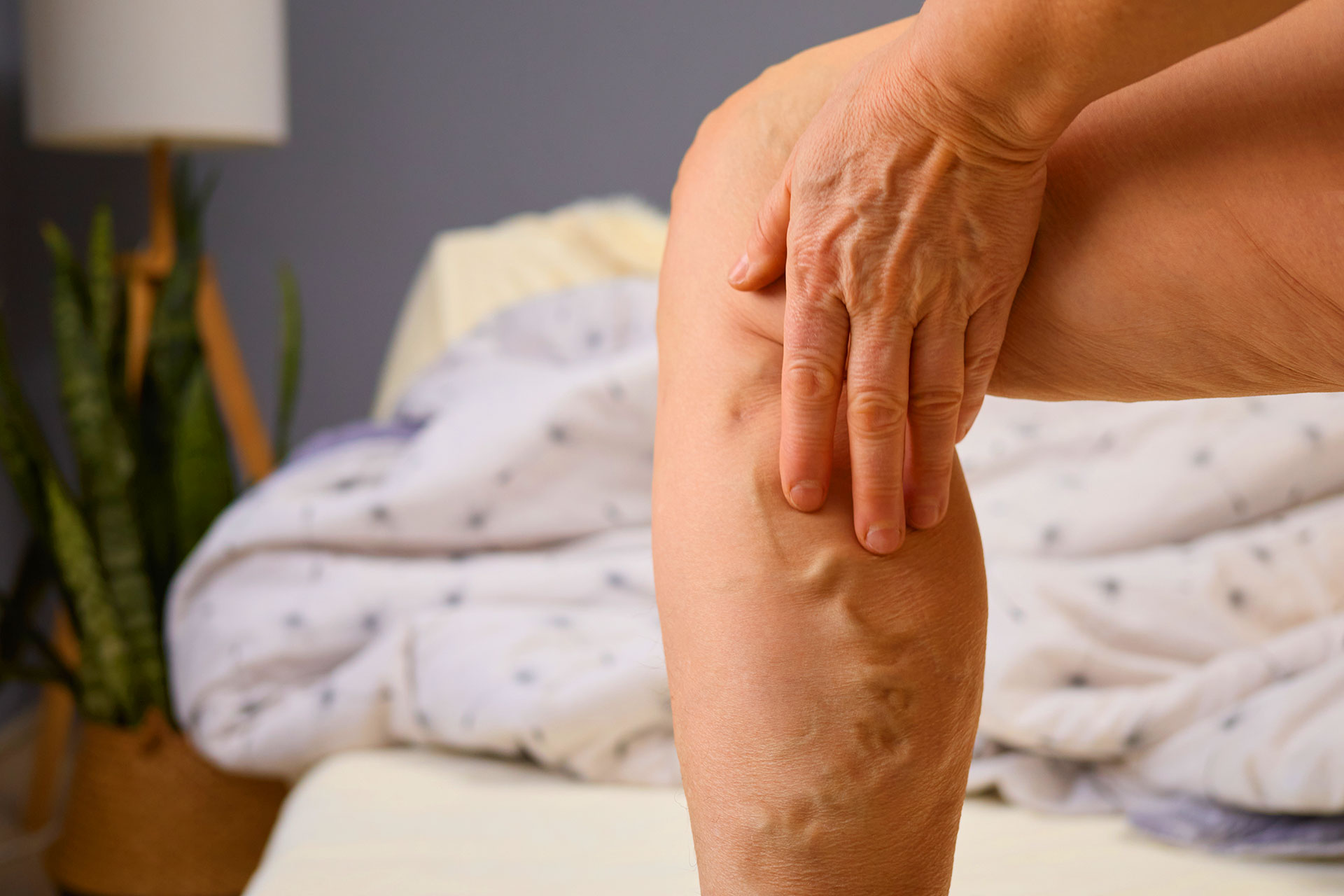
Varicose veins often present with visible symptoms, including twisted, bulging veins, leg heaviness, aching, and discomfort, especially after long periods of standing or sitting. Swelling and discoloration, such as dark purple spots, may also occur. In more advanced cases, skin changes or venous ulcers may develop.
The diagnostic process generally includes a physical examination, a review of medical and family history, and imaging tests to evaluate blood flow. Varicose veins develop when vein valves weaken, leading to blood pooling and vein enlargement. Hormonal changes, especially during pregnancy, can increase the likelihood of developing varicose veins.
If symptoms appear, using compression stockings, staying active, avoiding extended periods of sitting or standing, and consulting a medical professional can help manage the condition and prevent further complications.
Accurate diagnosis is crucial for effectively managing varicose veins. A physical examination, along with a detailed review of family history, helps identify risk factors and provides insight into the patient’s medical background. The causes and contributing factors of varicose veins include:
Doppler ultrasound is frequently used to diagnose varicose veins and assess blood flow. Physicians also evaluate changes in skin color, vein enlargement, the presence of ulcers, and signs of chronic venous insufficiency in addition to the patient’s symptoms.
The treatment for varicose veins varies based on the severity of the condition and the symptoms experienced. Common approaches include:
Maintaining proper blood circulation is key to preventing varicose veins and preserving overall vascular health. When varicose veins affect the blood vessels, they can disrupt normal circulation. Treatment options range from conservative measures, such as compression stockings and lifestyle changes, to advanced medical procedures for more severe cases.
Consulting a healthcare professional is essential to determine the most suitable treatment plan for each individual. The choice of treatment depends on factors such as the size and location of the veins, the symptoms experienced, and your overall health. A personalized approach ensures the most effective and targeted care for optimal results.