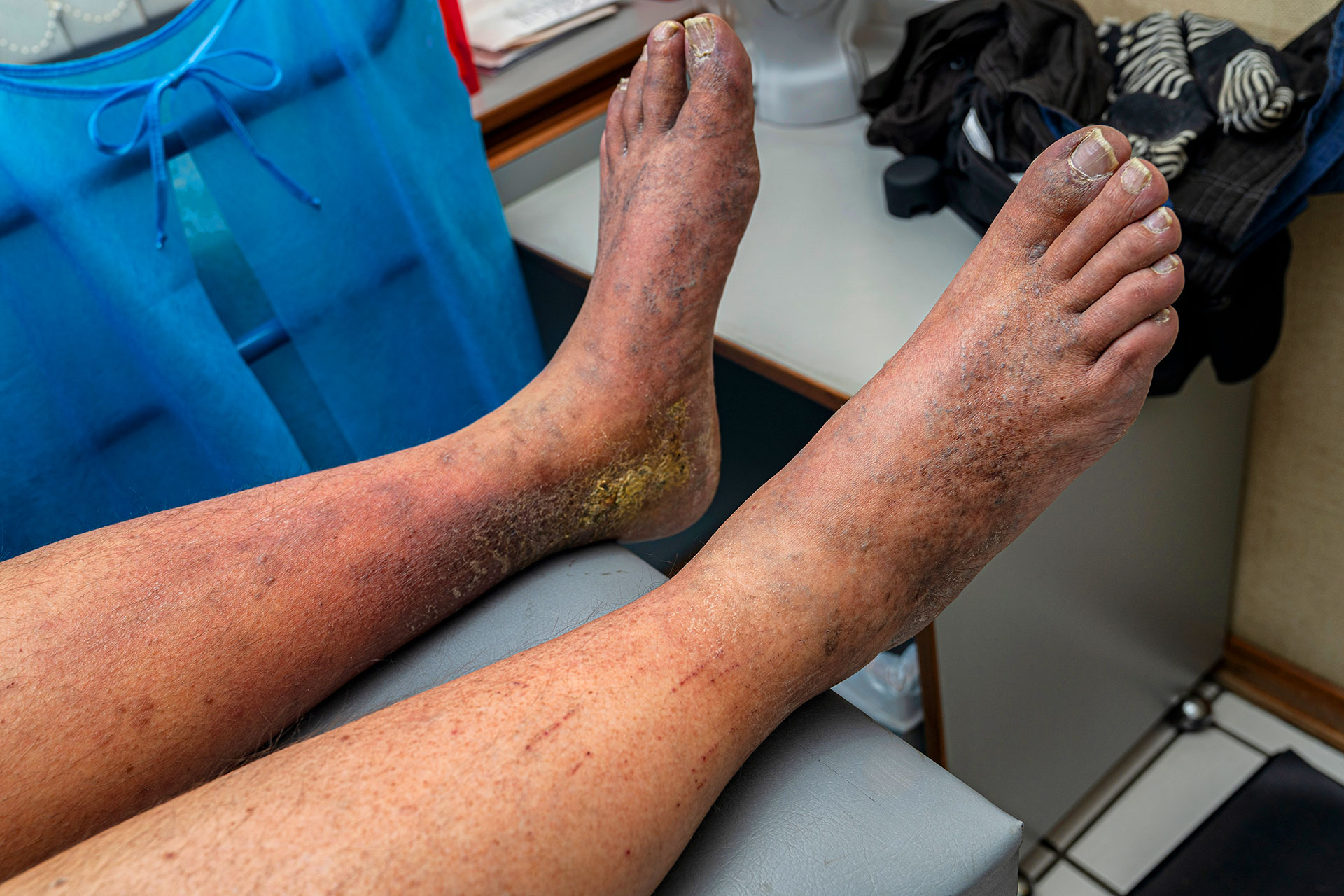
A complete diagnosis of chronic venous insufficiency includes reviewing the patient’s medical history and conducting a detailed physical examination of the legs. Doctors may ask about family history, lifestyle habits such as extended standing or sitting, and any associated symptoms.
During the physical exam, the doctor closely inspects and gently evaluates the legs to detect visible signs of vein disorders. Imaging tests may also be used to better assess blood flow.
Duplex ultrasound is an important diagnostic tool that shows blood flow in the veins. It helps detect damaged veins and evaluate the severity of the condition, supporting proper treatment decisions.
Knowing the risk factors is important for early detection and prevention efforts:
Balanced, fiber-rich diet, staying properly hydrated, and stopping smoking can all support stronger vascular health. Regular movement and avoiding long periods of sitting or standing also help improve circulation, especially when breaks are difficult.
Regular exercise supports overall blood flow, while maintaining a healthy weight lowers pressure on the veins and improves circulation. Raising the legs periodically can also help prevent blood pooling and lessen swelling.
Knowing the symptoms, risk factors, and care options for venous insufficiency is important for maintaining vascular health. By combining lifestyle adjustments, compression therapy, and, when necessary, medical procedures, individuals can improve blood flow and help avoid complications. If you suspect venous insufficiency, consult a healthcare professional for proper evaluation and a personalized care plan.