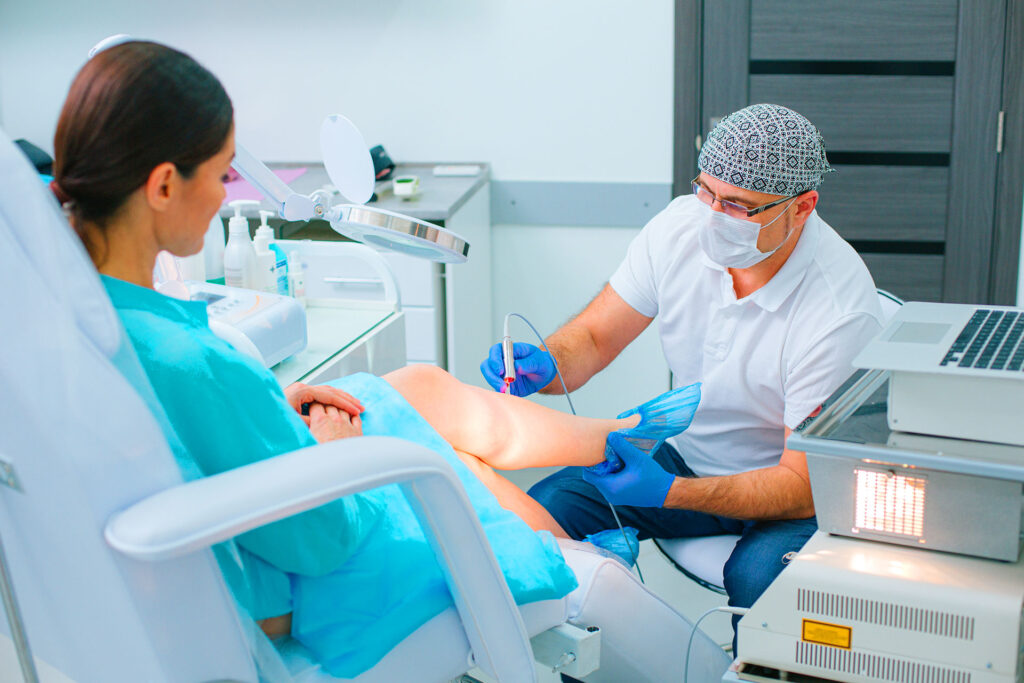
Vein disease is more widespread than many people think. If you’ve started noticing heavy legs, visible varicose veins, or ongoing swelling, visiting a vein clinic may be an important first step toward long-term relief. This guide explains who should seek evaluation, what happens during the assessment, and what treatment options may be available.
1 in 3
Americans over 45 live with some form of vein disease
90%
of vein treatments are minimally invasive and require little to no downtime
Most
cases are covered by insurance when treatment is medically necessary
Who Should Consider Visiting a Vein Clinic?
Your veins return blood to the heart using a network of one-way valves. When these valves become weak or stop working properly, blood can flow backward and collect in the lower legs, a condition called chronic venous insufficiency. A range of factors can increase the risk, including genetics, aging, previous blood clots, long periods of sitting or standing, obesity, and pregnancy.
Common Signs and Symptoms
Leg Heaviness
A lingering feeling of heaviness or fatigue in the legs, particularly after extended standing.
Leg Pain and Aching
A steady, aching pain in the calves or thighs that tends to intensify as the day goes on.
Night Cramps
Uncontrolled leg cramps at night, frequently associated with reduced or impaired venous circulation.
Swelling (Edema)
Swelling in the ankles and lower legs, especially more noticeable toward the end of the day.
Varicose Veins
Prominent, twisted veins that can be seen under the skin, commonly appearing on the legs.
Skin Changes
Skin changes such as discoloration, surface eczema, or, in more advanced cases, venous ulcers.
📌 Do Not Wait for Symptoms to Worsen
What Happens During Your Vein Clinic Visit?
A visit to a vein clinic follows a clear, step-by-step process that helps your physician fully assess your vein health before suggesting any treatment options.
Consultation with a Board-Certified Phlebologist
Your appointment starts with a detailed consultation with a vein specialist, also called a phlebologist. These doctors are trained in areas such as vascular surgery or cardiology, or are certified through the American Board of Venous and Lymphatic Medicine (ABVLM). Checking a provider’s credentials before your visit is always a good first step.
Medical History Review and Physical Examination
The specialist will review your medical history in detail, including your symptoms, daily habits, and family background of vein disease, followed by a physical examination of your legs. This process helps identify potential risk factors and guides the choice of appropriate diagnostic tests.
Vascular Duplex Ultrasound
In most cases, a registered vascular technologist performs a non-invasive duplex ultrasound of the legs. This imaging test visualizes the venous system, detects areas of valve failure and reflux, and assesses the severity of any insufficiency. It is advisable to choose clinics where sonographers are certified as Registered Vascular Technologists (RVT) through the American Registry for Diagnostic Medical Sonography (ARDMS).
Results Review and Personalized Treatment Plan
Once the tests are finished, your physician will go over the results with you and create a personalized treatment plan. The recommended approach depends on the size and location of the affected veins, the severity of your symptoms, and your individual goals. In most cases, treatments are done in-office and are covered by insurance when they are medically necessary.
🏅 ABVLM Certified
Available Vein Treatment Options
Modern vein clinics provide a variety of minimally invasive treatments for both medical and cosmetic vein concerns. Your specialist will choose the option that best matches your vein condition, anatomy, and treatment goals.
Endovenous Thermal Ablation
Ultrasound-Guided Foam Sclerotherapy
Surface Sclerotherapy
Frequently Asked Questions
Still have questions about what to expect at a vein clinic? Our specialists address the most frequently asked questions below.
In many cases, yes. When varicose veins lead to documented medical symptoms such as pain, swelling, or skin changes, treatment is often classified as medically necessary and covered by most major insurance plans. Cosmetic procedures, like surface sclerotherapy for spider veins, are usually not covered. The CURA team will check your insurance benefits before your appointment so you know what to expect in advance.
An initial consultation, which includes a physical examination and vascular ultrasound, usually lasts about 60 to 90 minutes. Treatment visits are generally shorter. Most in-office procedures, such as thermal ablation or sclerotherapy, take around 30 to 60 minutes to complete, and patients are typically able to return to light daily activities the same day.
Not at all. A vascular duplex ultrasound is entirely non-invasive and painless. A small handheld probe is gently moved over the surface of your leg to create images of the veins beneath the skin. There are no needles, no radiation, and no special preparation needed beforehand. Most patients describe it as similar to a routine imaging test.
When choosing a vein specialist, look for physicians who are board-certified through the American Board of Venous and Lymphatic Medicine or who have training in vascular surgery or cardiology. For ultrasound evaluations, the Registered Vascular Technologist (RVT) credential from the American Registry for Diagnostic Medical Sonography is considered the industry standard.
At CURA Vein Centers, both the treating physicians and ultrasound technicians meet the appropriate professional certification requirements.
This depends on the extent and severity of your vein disease. Some patients reach their treatment goals in a single session, while others with more widespread venous insufficiency may need a series of procedures spaced over several weeks. During your consultation, your physician will provide a clear, personalized timeline based on your ultrasound results and symptom pattern.
Treated veins do not return once they have been closed. However, vein disease is a chronic condition, meaning new problem veins can still develop over time, especially if underlying risk factors like genetics, prolonged standing, or hormonal changes remain present.
Adopting supportive habits such as wearing compression stockings, maintaining a healthy body weight, and staying physically active can help slow the progression of new vein disease after treatment.